Guide B-717
Jason L. Turner
College of Agricultural, Consumer and Environmental Sciences, New Mexico State University
Extension Horse Specialist, Department of Extension Animal Sciences and Natural Resources, New Mexico State University. (Print Friendly PDF)

Introduction
The first reported case of vesicular stomatitis (VS) in the United States was in 1916. Since then there have been sporadic outbreaks of the disease in North America, most commonly occurring in the southwestern U.S. Vesicular stomatitis virus (VSV) is endemic throughout Mexico, Central America, and South America. Outbreaks typically occur in the southwestern U.S. beginning in late spring or early summer. These outbreaks normally continue through late fall, progressing northward often along riverways and valleys. The outbreaks subside after freezing temperatures kill the insect vectors that transmit VSV. However, the virus may overwinter for a year or two, allowing re-emergence in the spring.
Although horses are not known to be infected by foot and mouth disease (FMD), the clinical signs of VS are indistinguishable from those of FMD. In order to protect animal health interests across the U.S., VS is a reportable disease, which means veterinarians have a duty to report suspect VS cases to state and federal animal health authorities. While VSV primarily affects equids, cattle, and swine, it can also occur in sheep, goats, llamas, alpacas, and a variety of wild vertebrates. As a zoonotic disease, VSV can infect humans and cause flu-like symptoms, so it is important that people handling infected horses practice proper biosecurity to protect themselves as well as other animals.
Clinical Signs
The incidence of disease is highly variable, ranging from 5% to more than 90% in exposed populations. The incubation period, or time from exposure to presence of clinical symptoms, usually ranges from two to eight days. The clinical symptoms (Figures 1A–1C) of VS include vesicles, papules, erosions, and ulcerations that occur primarily in and around the mouth. However, lesions can occur in the ears, on the coronary band of the feet, on the teats and udder, and on the prepuce (sheath) (Figures 2A–2D). The predominant sites affected are likely due to differences in the feeding preferences of the insect vectors. If initial stages of the disease go unnoticed, subsequent lesions may appear as crusting scabs on the muzzle, lips, belly, sheath, and udder.
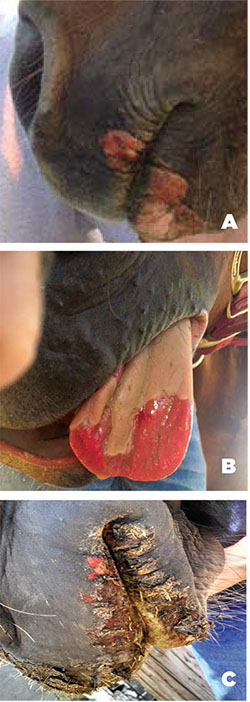
Figures 1A–1C. Vesicles and erosions on the mouth (A), tongue (B), nose, and lips (C) of horses with VS. (Photos by Colorado Department of Agriculture. Used with permission.)
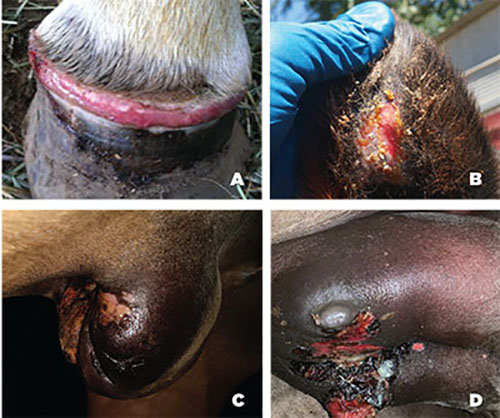
Figures 2A–2D. Lesions on the coronary band (A), ears (B), sheath (C), and teats (D) of horses with VS. (Photos by Colorado Department of Agriculture. Used with permission.)
Although fever may accompany the initial infection, this may disappear before the presence of vesicles prompts examination of the animal. Drooling and excess salivation are typically the first symptoms noticed. Upon closer examination, there may be blanched areas and the characteristic vesicles or blisters. As these vesicles rupture, they may cause large denuded areas in the oral mucosa. These lesions are quite painful and can cause loss of appetite and/or refusal to drink water. Lesions on the feet can cause lameness, and sores on the teats can lead to mastitis through secondary bacterial infections. Unless complications or secondary bacterial infections develop, equids normally recover from VS within two to three weeks.
Disease Transmission
Although there have been recent improvements in our understanding of how VSV is transmitted, many specific details concerning disease transmission are still unknown. There is compelling evidence that insect vectors (primarily sandflies, black flies, and biting midges) introduce VSV into populations of domestic animals. While black flies are believed to be the primary vector in the western U.S., Table 1 lists several insects that are capable of harboring VSV. Once animals develop lesions, insects may become infected by feeding on virus within the lesions or contaminated secretions. Infected black flies can transmit VSV to other black flies while feeding at the same time, even on an uninfected host. Furthermore, VSV has been shown to be passed from parent to offspring (transovarial transmission) in sandflies, black flies, and possibly Culicoides midges. Experts believe that this mode of transmission may be responsible for the spring re-emergence of VSV seen in some multi-year outbreaks.
|
Table 1. Insects from which Vesicular Stomatitis Virus |
|
|
Genus |
Common name |
|
Lutzomyia |
Sandfly |
|
Simulium |
Black fly |
|
Culicoides |
Biting midge |
|
Tabanus |
Horse fly |
|
Chrysops |
Deer fly |
|
Aedes |
Mosquito |
|
Culex |
Mosquito |
|
Musca |
House fly |
|
Hippelates |
Eye gnat |
|
Modified from McCluskey (2007). |
|
Once VSV has been introduced within a herd, saliva from infected animals is contaminated with VSV and can infect others. The VSV present in saliva has been reported to survive on equipment and feedstuffs for three to four days. Under ideal laboratory conditions, the virus has been shown to persist for three to four weeks.
Treatment
While there is no specific treatment for the virus, supportive therapy is recommended to help the infected equine recover. Cleaning the lesions with a mild antiseptic solution, such as chlorhexidine diluted in water, can promote healing and reduce secondary bacterial infections. If the lesions cause reduced feed or water intake, feeding soft feedstuffs or intravenous fluids may be recommended by the attending veterinarian. Anti-inflammatory medications may also be prescribed to minimize discomfort, swelling, lameness, and pain in severe cases.
Preventive Measures and Isolation Protocols
Since there is no commercially available vaccine for VSV licensed in the U.S., minimizing the risk of exposure for your horse is the best preventive measure. The following suggestions can help reduce the incidence of VS:
- Maintain an insect control program. Removing stagnant water sources, muddy areas, and manure can reduce the breeding areas of the insects that transmit VSV. Routine use of a pyrethrin-based insect repellent or insecticide on your horse, especially inside the ears where black flies tend to feed, can also reduce the risks from insects. Fly sheets, screens, and masks (with ears) may also help.
- Stabling horses rather than leaving them on pasture during an outbreak has been shown to reduce the risk of VS. This is likely due to the larger population of insect vectors that reside on pastures, especially near water sources (streams, dirt tanks or ponds, irrigation canals, etc.).
- Routinely inspect your horses for signs of VS and isolate suspect animals from the rest of the herd. Once the symptoms develop in a herd, the infected animals quickly pass it to others through direct contact with each other as well as vesicular fluid that contaminates equipment (feed troughs, water troughs and buckets, hay feeders, bits, halters, other tack, etc.) and other surfaces (trailer mangers, tie rails, etc.).
- Use individual rather than communal feeders, waterers, bits, etc.
- Practice good sanitation and disinfection to help reduce the spread of VS. Sunlight is known to kill VSV, and commercial disinfectants, such as chlorine bleach (0.645%), are also effective.
- Isolate new horses for at least 21 days before turning them in with other resident animals.
- Ask your farrier and other equine professionals that visit your farm or come in contact with your horses to practice good biosecurity when they arrive so that they do not inadvertently spread disease from one horse (or facility) to the next.
- If traveling with your horse, prepare what you will need to practice good biosecurity when you arrive at the location. Use your own equipment and buckets. It is better to let water run from the end of the hose into a bucket or trough without submerging the hose into the water since this is a better biosecurity practice. Disinfect your stall area. Above all, minimize direct contact with other animals.
- If a farm has suspect VS cases, people should practice good biosecurity to prevent transmission to non-infected animals. This includes handling and caring for suspect or infected animals after all the normal animals have been cared for. Handlers should then shower, change clothes, and disinfect equipment. Wearing disposable gloves and washing hands after handling suspect or infected animals is also recommended.
Just because a horse has vesicles in the mouth does not mean they have VS. Adverse reactions to non-steroidal anti-inflammatory medications or other drugs as well as irritation of the oral mucosa due to certain plants in the hay may cause lesions similar to those seen with VS. Your veterinarian or other animal health officials will collect samples from the horse for laboratory testing to confirm the diagnosis with VSV. If the horse is confirmed positive for VSV infection, then the premise will be quarantined with movement restrictions. Quarantine periods may range from at least 14 days from the onset of lesions in the last affected animal on the premise to at least 21 days after all lesions are healed. Your veterinarian can give you specific details on the quarantine restrictions and timeline for your premise.
Conclusion
Good communication with your veterinarian and animal health officials is important in dealing with disease outbreaks such as VS. The references below are excellent sources of more specific information on VS. It is important to be aware of what documents are required for transporting equines within a state as well as across state borders, especially when a disease outbreak occurs. You can learn more about these requirements in NMSU Extension Guide B-708, Documents Required to Transport Horses in New Mexico (https://pubs.nmsu.edu/_b/B708/). For current recommendations and regulatory information on VS, you can visit the New Mexico Livestock Board web page (www.nmlbonline.com), or contact the Office of the State Veterinarian:
300 San Mateo Blvd. NE, Ste. 1000
Albuquerque, NM 87108-1500
Phone: 505-841-6161
Fax: 505-841-6160.
References
Colorado Department of Agriculture. n.d. Vesicular stomatitis virus (VSV). https://drive.google.com/file/d/1AWC-7db4_vhlnNqT7TZDQ7Knxj1GoGfy/view
Larson, E. 2014, September 11. Vesicular stomatitis: What you need to know. https://thehorse.com/149704/vesicular-stomatitis-what-you-need-to-know
McCluskey, B.J. 2007. Vesicular stomatitis. In D.C. Sellon and M.T. Long (Eds.), Equine Infectious Diseases, 1st ed. (pp. 219–225). St. Louis: Saunders Elsevier.
New Mexico Livestock Board. 2019. Vesicular stomatitis. https://www.nmlbonline.com/documents/Vesicular%20Stomatitis%20Factsheet%20June%202019.pdf
Pelzel-McCluskey, A. 2016. Vesicular stomatitis in horses. https://aaep.org/horsehealth/vesicular-stomatitis-horses
Spickler, A.R. 2016. Vesicular stomatitis. https://www.cfsph.iastate.edu/Factsheets/pdfs/vesicular_stomatitis.pdf
The Merck Veterinary Manual. n.d. Whitehouse Station, NJ: Merck & Co., Inc. https://www.merckvetmanual.com
For Further Reading
B-707: Evaluation of Equine Hoof Care
https://pubs.nmsu.edu/_b/B707/
B-708: Documents Required to Transport Horses in New Mexico
https://pubs.nmsu.edu/_b/B708/
B-708: Documentos requeridos para el transporte de caballos en Nuevo México
https://pubs.nmsu.edu/_b/B708sp/
B-716: Equine Herpesvirus in Horses
https://pubs.nmsu.edu/_b/B716/

Jason L. Turner is Associate Professor and Extension Horse Specialist. Jason was active in 4-H and FFA while growing up in Northeastern Oklahoma. His M.S. and Ph.D. studies concentrated on equine reproduction, health, and management. His Extension programs focus on proper care and management of the horse for youth and adults.
To find more resources for your business, home, or family, visit the College of Agricultural, Consumer and Environmental Sciences on the World Wide Web at pubs.nmsu.edu.
Contents of publications may be freely reproduced, with an appropriate citation, for educational purposes. All other rights reserved. For permission to use publications for other purposes, contact pubs@nmsu.edu or the authors listed on the publication.
New Mexico State University is an equal opportunity/affirmative action employer and educator. NMSU and the U.S. Department of Agriculture cooperating.
April 2020 Las Cruces, NM